Answered step by step
Verified Expert Solution
Question
1 Approved Answer
2. Options: Contractual adjustments, Capitation fees, Charity care, Diagnosis-related groups, Prospective payment system, Health maintenance organizations, Performance indicator, Third-party payor For each of the following
2.
Options: Contractual adjustments, Capitation fees, Charity care, Diagnosis-related groups, Prospective payment system, Health maintenance organizations, Performance indicator, Third-party payor
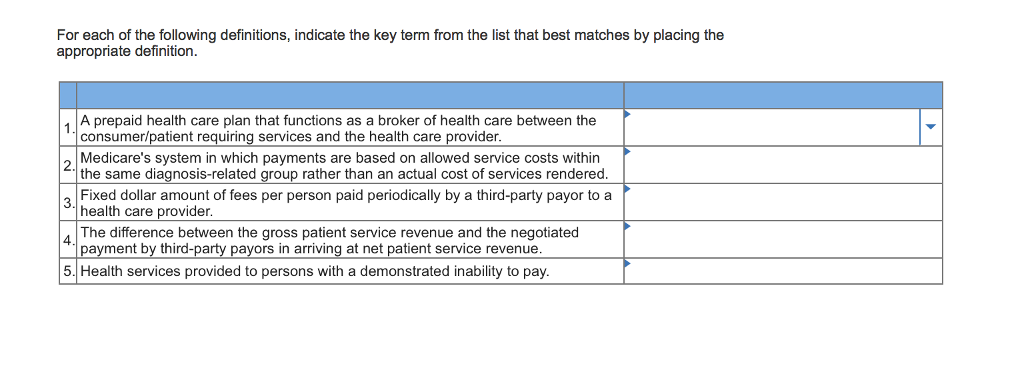
For each of the following definitions, indicate the key term from the list that best matches by placing the appropriate definition. A prepaid health care plan that functions as a broker of health care between the consumer/patient requiring services and the health care provider Medicare's system in which payments are based on allowed service costs within the same diagnosis-related group rather than an actual cost of services rendered. 3 Fixed dollar amount of fees per person paid periodically by a third-party payor to a 4. The difference between the gross patient service revenue and the negotiated 5. Health services provided to persons with a demonstrated inability to pay. health care provider payment by third-party payors in arriving at net patient service revenueStep by Step Solution
There are 3 Steps involved in it
Step: 1

Get Instant Access to Expert-Tailored Solutions
See step-by-step solutions with expert insights and AI powered tools for academic success
Step: 2

Step: 3

Ace Your Homework with AI
Get the answers you need in no time with our AI-driven, step-by-step assistance
Get Started


